(NewsUSA) - Like many veterans, Brian Owens, 53 from Kentucky, knows all too well that the invisible burdens of military service can linger long after the uniform comes off. For Brian, a U.S. Marine Corps veteran, it was his heart that felt the ongoing impacts the most.
- Like many veterans, Brian Owens, 53 from Kentucky, knows all too well that the invisible burdens of military service can linger long after the uniform comes off. For Brian, a U.S. Marine Corps veteran, it was his heart that felt the ongoing impacts the most.
Veterans face an increased risk of developing hypertension, commonly known as high blood pressure, a condition that affects an estimated 37% of the U.S. veteran population.1 Research from a large cohort study found that both combat exposure and combat injury were associated with higher odds of developing hypertension.2 For Brian, this is significant as men are already more likely to develop high blood pressure - 50.8% of adult men compared to 44.6% of women - and face greater cardiovascular risk over time.3
Treating hypertension early on is essential as the condition can increase the risk of heart attack, stroke, and other health concerns if left untreated.4,5 Brian’s treatment journey started like most do, being prescribed medication for high blood pressure and making changes to his diet and exercise routine. For Brian, the medication was helpful at first, but over time, his blood pressure increased, even with multiple prescriptions. “I was on five or six different medications at one point,” Brian recalls. "I was doing what I was supposed to, but I wasn’t getting better.”
Brian’s experience reflects a wider problem: controlling the “silent killer” is often elusive, and medication is not always enough. In fact, up to 50% of patients can’t maintain a routine to take medication within one year.6,7
After years of trying and seeing little progress, Brian started to feel helpless - like blood pressure control was out of reach. While working at Norton Healthcare, Brian ran into Dr. Matthew Sousa, an interventional cardiologist, who helped him seek answers for his uncontrolled high blood pressure. Dr. Sousa and Debbie Davis, a nurse manager at Norton Healthcare, helped him learn more about his treatment options and ultimately decide on a path forward.
“After telling Debbie and Dr. Sousa my story and concerns, they asked if I’d be open to a new procedure that could help,” Brian said. After discussing his options with his doctor and seeing if he would be a good candidate, Brian decided to move forward with a minimally invasive treatment called the SymplicityTM blood pressure procedure, which uses radiofrequency energy to calm overactive nerves near the kidneys that can contribute to high blood pressure.8
The Symplicity blood pressure procedure, which uses the Symplicity Spyral renal denervation system, can help reduce blood pressure numbers when other options, such as lifestyle changes and medications, haven’t worked. In fact, at three years, the average number of patients taking medication saw an 18.5 mmHg reduction in office blood pressure, although results may vary.9 The procedure may deliver sustained blood pressure reduction.**10, 11
Since having the Symplicity blood pressure procedure, Brian has experienced a reduction in his blood pressure.*** Now, Brian is sharing his story in hopes of helping others, especially fellow veterans. “It’s something a lot of veterans are dealing with, but don’t talk about,” he said. “If my experience can help someone else ask the right questions or explore new options, it’s worth it.”
Between volunteering with Toys for Tots, raising two daughters, and staying active through competitive shooting, Brian is embracing a new chapter with renewed energy and a healthier outlook on life.
To learn more about renal denervation and the Symplicity blood pressure procedure, visit beyondHBP.com. Risks associated with the Symplicity blood pressure procedure include, but are not limited to, pain and bruising. If you have high blood pressure, talk to your doctor about treatment options.
*Brian has received compensation in the past from Medtronic for sharing his experience with the Symplicity blood pressure procedure.
**Data available through three years.
***This patient testimonial is an individual’s experience and opinion. Not every person will experience the same results. The Symplicity procedure has known risks that should be considered in relation to the potential benefits of the procedure. People with higher blood pressure before the procedure may see greater reductions in blood pressure and a decrease in the need for blood pressure medication following the procedure. However, individual results may vary.
1 American Heart Association Newsroom. Joining Forces to Address Hypertension Among Veterans in Las Vegas. https://newsroom.heart.org/local-news/joining-forces-to-address-hypertension-among-veterans-in-las-vegas. Published March 8, 2023
2. Howard, J. T., Stewart, I. J., Kolaja, C. A., Sosnov, J. A., Rull, R. P., Torres, I., Janak, J. C., Walker, L. E., Trone, D. W., & Armenta, R. F. (2020). Hypertension in military veterans is associated with combat exposure and combat injury. Journal of hypertension, 38(7), 1293–1301. https://doi.org/10.1097/HJH.0000000000002364
3 Fryar, C. D., Kit, B. K., Carroll, M. D., & Afful, J. (2024, October). Hypertension prevalence, awareness, treatment, and control among adults aged 18 and over: United States, August 2021–August 2023 (NCHS Data Brief No. 511). National Center for Health Statistics. https://www.cdc.gov/nchs/data/databriefs/db511.pdf
4 Jones DW, et al. 2025 AHA/ACC/AANP/AAPA/ABC/ACCP/ACPM/AGS/AMA/ASPC/NMA/PCNA/SGIM Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol. 2025 Nov 4;86(18):1567-1678.
5 High blood pressure dangers: Hypertension’s effects on your body. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/highblood-pressure/in-depth/high-blood-pressure/art-20045868. Accessed Oct 16, 2024.
6 Jung O, Gechter JL, Wunder C, et al. Resistant hypertension? Assessment of adherence by toxicological urine analysis. J Hypertens. 2013 Apr;31(4):766-74.
7 Berra E, Azizi M, Capron A, et al. Evaluation of Adherence Should Become an Integral Part of Assessment of Patients With Apparently Treatment-Resistant Hypertension. Hypertension. 2016 Aug;68(2):297-306.
8 Coates P, Tunev S, Trudel J, Hettrick DA. Time, Temperature, Power, and Impedance Considerations for Radiofrequency Catheter Renal Denervation. Cardiovasc Revasc Med. September 2022;42:171–177.
9 Kandzari, DE. SPYRAL HTN-ON MED 3 Year Data. Transcatheter Cardiovascular Therapeutics (TCT) conference. October 2025.
10 Mahfoud F, Kandzari DE, Kario K, et al. Long-term efficacy and safety of renal denervation in the presence of antihypertensive drugs (SPYRAL HTN-ON MED): a randomised, sham-controlled trial. Lancet. April 9, 2022;399(10333):1401–1410.
11 Mahfoud F, Mancia G, Schmieder R, et al. Blood pressure and MACE reductions after renal denervation: 3-year Global Symplicity Registry results. Presented at PCR e-Course 2022."
US-SE-2500758 v 3.0
©2026 Medtronic. Medtronic, Medtronic logo, and Engineering the extraordinary are trademarks of Medtronic. All other brands are trademarks of a Medtronic company
Important Safety Information
The Symplicity™ blood pressure procedure (BPP) is a minimally invasive procedure approved to help lower high blood pressure. The procedure is approved as a complement to treatments you may already be trying, such as lifestyle modifications and high blood pressure medications that might not be adequately controlling your blood pressure.
Receiving the Symplicity BPP should be based on a joint decision between you and your doctor. Consider the benefits and risks of the device and procedure. Please talk to your doctor to decide whether or not the Symplicity BPP is right for you.
If you have a pacemaker or an ICD, your doctor will follow up with steps to take ahead of the procedure if you decide it is right for you.
At the time of your procedure, your doctor may detect certain anatomical conditions (e.g., your blood vessels are too big or too small) that do not allow the blood pressure procedure to continue.
You should not receive the procedure if you cannot tolerate medications that are required for the procedure, like atropine, nitroglycerin, systemic blood thinners, or certain pain medications. These medications are to help you in case your heart rate drops too low, you experience pain, or your blood vessels tighten during the procedure. You should not receive the procedure if you are pregnant.
The Symplicity BPP has not been studied in patients: • Who are breastfeeding • Who are under 18 years old • Who have isolated systolic hypertension (only the “top number” of your blood pressure is high) • Who have secondary causes of high blood pressure
• Who have had a renal stent placed less than 3 months prior to the procedure • Who had a prior minimally invasive treatment in their renal arteries (stenting, angioplasty, or prior renal denervation)
Potential risks of the Symplicity BPP (note that you may experience other problems that have not been previously observed with this procedure): • Allergic reaction to the imaging solution • Damage to your arteries • Future narrowing of your arteries • Arterio-enteric fistula (an abnormal connection between your aorta and your gastrointestinal tract) • AV fistula (an irregular connection between an artery and a vein) • Bleeding or blood clots • Bruising where the device enters your body (mild or severe) • Cardiac arrest or heart attack • Death • Deep vein thrombosis • Swelling • Slow heart rate • Infection • Low or high blood pressure • Damage to your kidneys that may cause one or both to stop working • Nausea or vomiting • Peripheral ischemia (lack of blood supply to your limbs) • Pulmonary embolism (a sudden block in your arteries that send blood to your lungs) • Pseudoaneurysm (blood collecting on the outside of a vessel wall causing a balloon-like widening) • Pain or discomfort • Skin burns from the failure of the equipment during the procedure • Exposure to radiation • Stroke
For further information, please call and/or consult Medtronic at 800-633-8766 or the Medtronic website at medtronic.com.
 - Better brain health doesn't have to be complicated, and you can start now. Achievable, practical steps can make a real difference at any age. It’s never too late, or too soon, to shape your brain health. Research from the Alzheimer's Association shows that everyday habits, including how you move, what you eat, and how you engage your mind, can help you live better now, protect your memory over time, and potentially help reduce your risk of dementia.
- Better brain health doesn't have to be complicated, and you can start now. Achievable, practical steps can make a real difference at any age. It’s never too late, or too soon, to shape your brain health. Research from the Alzheimer's Association shows that everyday habits, including how you move, what you eat, and how you engage your mind, can help you live better now, protect your memory over time, and potentially help reduce your risk of dementia.

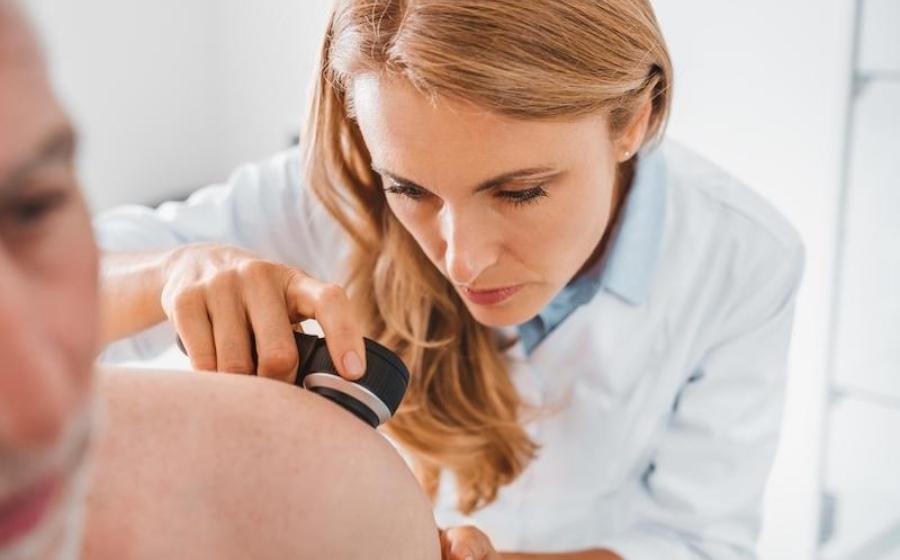
 - When faced with a skin cancer diagnosis, Americans are no longer passive recipients of care. A recent survey of patients confronting treatment decisions shows a clear shift toward empowered, informed decision-making, with cure rates, avoidance of surgery, and cosmetic outcomes topping the list of concerns – often outweighing even a doctor's recommendation.
- When faced with a skin cancer diagnosis, Americans are no longer passive recipients of care. A recent survey of patients confronting treatment decisions shows a clear shift toward empowered, informed decision-making, with cure rates, avoidance of surgery, and cosmetic outcomes topping the list of concerns – often outweighing even a doctor's recommendation.
 - As warm weather approaches, it’s time to spread the word about spreading sunscreen.
- As warm weather approaches, it’s time to spread the word about spreading sunscreen. - For decades, a quiet “third party” has sat in exam rooms across America: the computer screen. Patients have grown used to seeing the back of their doctor’s head—eyes fixed on a keyboard or tablet instead of on them—as notes are diligently entered.
- For decades, a quiet “third party” has sat in exam rooms across America: the computer screen. Patients have grown used to seeing the back of their doctor’s head—eyes fixed on a keyboard or tablet instead of on them—as notes are diligently entered.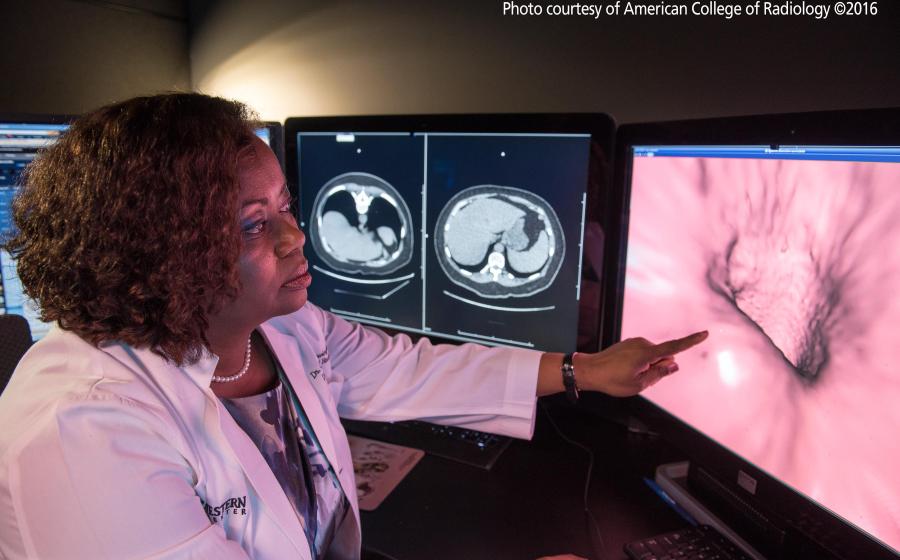
 - Expanded Coverage for Less-Invasive Tests Can Help
- Expanded Coverage for Less-Invasive Tests Can Help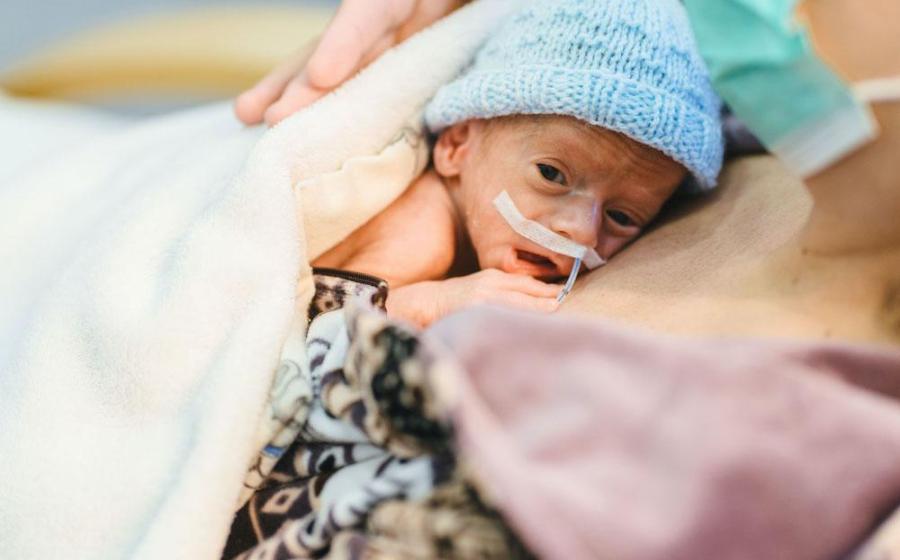
 - Premature babies face unique challenges from the moment they arrive. Born weeks or months before their bodies are fully developed, these fragile infants need every advantage to grow strong and healthy. The good news? Research shows that the right nutrition can help improve both their immediate health and their development years down the road.
- Premature babies face unique challenges from the moment they arrive. Born weeks or months before their bodies are fully developed, these fragile infants need every advantage to grow strong and healthy. The good news? Research shows that the right nutrition can help improve both their immediate health and their development years down the road.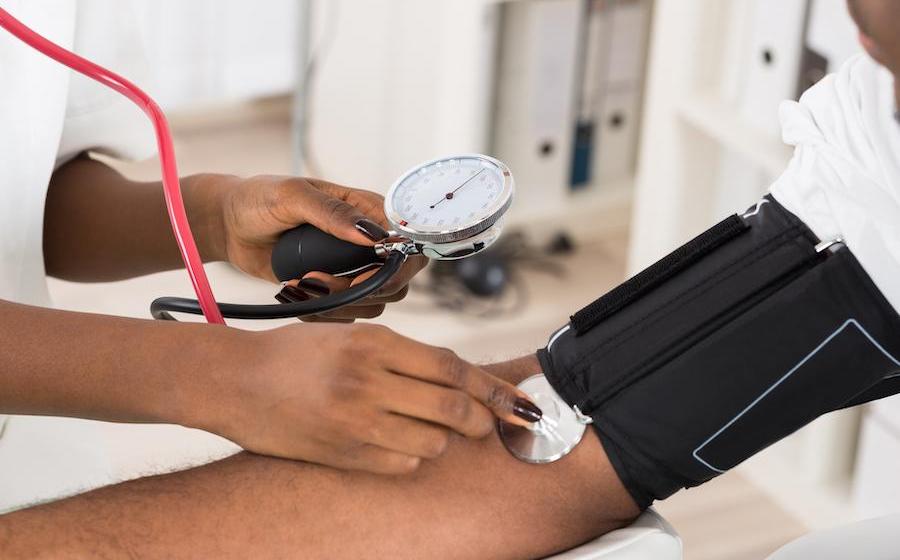
 - Like many veterans, Brian Owens, 53 from Kentucky, knows all too well that the invisible burdens of military service can linger long after the uniform comes off. For Brian, a U.S. Marine Corps veteran, it was his heart that felt the ongoing impacts the most.
- Like many veterans, Brian Owens, 53 from Kentucky, knows all too well that the invisible burdens of military service can linger long after the uniform comes off. For Brian, a U.S. Marine Corps veteran, it was his heart that felt the ongoing impacts the most.  -
-  As you set New Year’s resolutions, add one that takes just minutes and can make a real difference: protect your skin and get suspicious spots checked. Skin cancer is prevalent, but when caught early, it’s also highly treatable. Here are 10 facts and tips to start the year smarter about prevention and options.
As you set New Year’s resolutions, add one that takes just minutes and can make a real difference: protect your skin and get suspicious spots checked. Skin cancer is prevalent, but when caught early, it’s also highly treatable. Here are 10 facts and tips to start the year smarter about prevention and options.
 - Chilly December air can make for an ideal time to get your fitness routine started. That’s because seasonal changes naturally affect our bodies and habits.
- Chilly December air can make for an ideal time to get your fitness routine started. That’s because seasonal changes naturally affect our bodies and habits.
 - Obesity is a chronic disease affecting over 100 million Americans. Despite its prevalence and serious health consequences, widespread insurance barriers limit access to FDA-approved GLP-1 treatments.
- Obesity is a chronic disease affecting over 100 million Americans. Despite its prevalence and serious health consequences, widespread insurance barriers limit access to FDA-approved GLP-1 treatments.



